Why Templates
Don't Work
Template-based EMRs are rigid, cumbersome, frustrating to use, and limit your freedom to practice medicine your own way. Even worse, templates can increase your medical liability and your claim denials. You don't have to settle for template software. There's a better way.

Problem 1
Template-based software assumes that the template manufacturers knows more about your practice than you do.
This means that you have to sort through lists in order to make the template fit each encounter.
The best medicine is based on your personal experience, your individual style, and your own thinking process. Medicine is an art as well as a science.

Problem 2
Templates do not produce quality data.
Selecting data from lists forces you to sacrifice quality time with patients for data entry. This tension is reflected in the quality of the data that is produced.
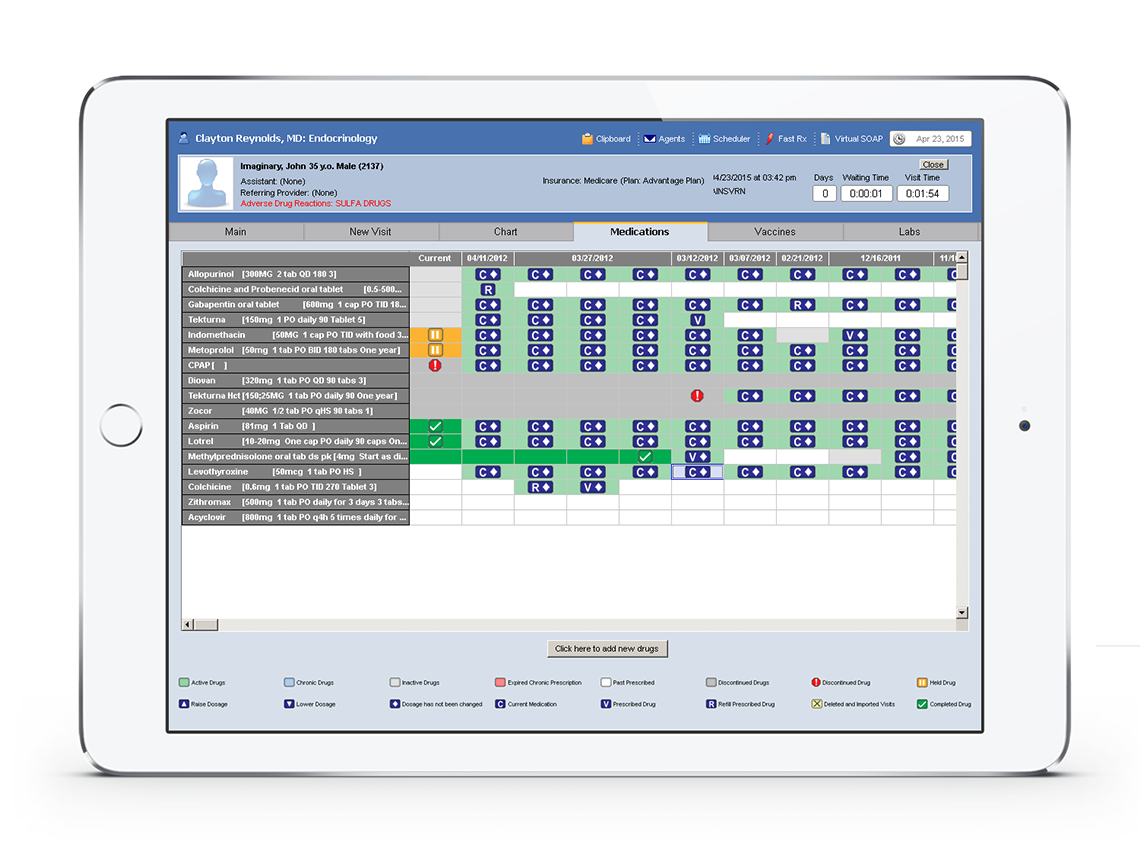
Problem 3
Templates increase your medical liability as well as your clinic's Medicare claim denials.
Templates do not qualify as sufficient documentation to receive Medicare payments.
Inappropriate and excessive alert systems also de-sensitize clinicians to alerts, leading them to ignore the truly important ones.
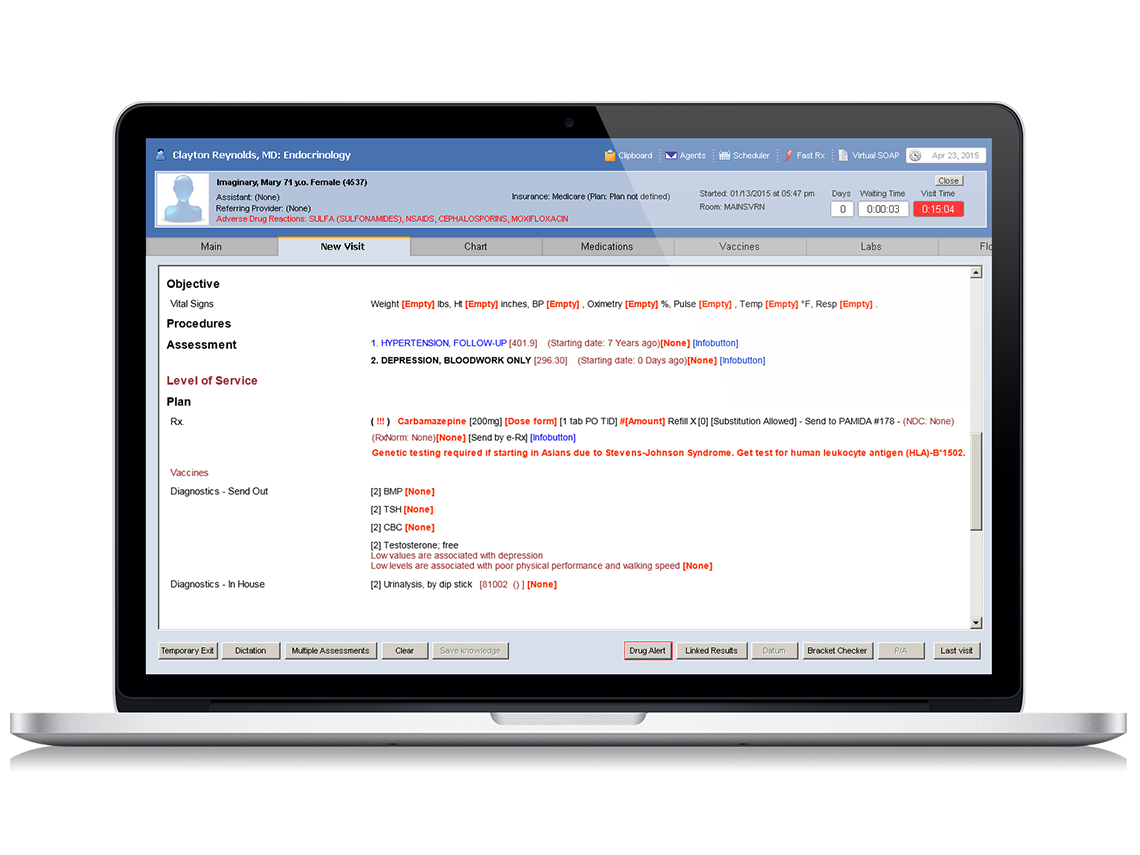
The myth of "Smart Templates"
Despite today's claims of "smart templates," and "templates that save," the constant editing of inflexible templates is cumbersome and time-consuming.
Fitting your patient into a template mold is not what medicine is about, and it's no way to practice your art.
The truth is that templates limit you.
We have a far better answer to Electronic Medical Records.
Learn more about the problems of Templates
